What Is Steatosis?
Steatosis, commonly known as fatty liver disease, is a condition in which excess fat builds up in the liver. It affects nearly 1 in 4 adults globally and often progresses silently. Though the liver naturally contains small amounts of fat, when more than 5–10% of its weight is fat, it’s considered steatotic. If left unaddressed, steatosis can lead to inflammation, scarring (fibrosis), cirrhosis, or even liver failure.
There are two main types:
- Non-Alcoholic Fatty Liver Disease (NAFLD): Linked to diet, lifestyle, insulin resistance, and obesity.
- Alcoholic Fatty Liver Disease (AFLD): Caused by excessive alcohol use.
While some people with steatosis experience no symptoms, others may develop signs of liver distress or feel fatigued. Importantly, steatosis is often reversible with early intervention, diet shifts, and movement.
How Steatosis Develops
The liver plays a vital role in breaking down fats, filtering toxins, and metabolizing nutrients. In steatosis, this system gets overwhelmed. Fat begins to accumulate inside liver cells (hepatocytes), interfering with their function. Over time, the liver becomes inflamed (steatohepatitis), then scarred (fibrosis), and in severe cases, may lose function altogether.

Steatosis Symptoms
Many people with fatty liver disease don’t notice symptoms until liver function is already impaired. That’s why routine blood tests and imaging are important, especially if you are at risk.

Abdominal Pain
A dull ache or fullness on the right side of the abdomen is common. This discomfort may come and go or worsen after eating.

Fatigue
Persistent, unexplained tiredness can occur as liver function declines. Your liver helps regulate energy levels, so a sluggish liver can leave you feeling wiped out.
Elevated Enzymes
Lab tests might reveal elevated ALT or AST levels, which are early signs of liver inflammation or injury—even before you feel sick.

🌙 Sleep Disturbance
Poor liver detoxification at night can interfere with sleep cycles, causing restlessness or waking between 1–3 a.m.

Shortness Of Breath
In more advanced cases, steatosis can lead to fluid buildup in the abdomen (ascites) or legs (edema), and even shortness of breath.
Fatty liver disease develops from a combination of lifestyle, genetic, metabolic, and environmental factors:
Rapid weight loss or starvation – Can paradoxically overload the liver with fat.

Excess sugar and refined carbohydrates – Fructose and white starches increase fat storage in the liver.

High alcohol intake – Alcohol disrupts fat metabolism and increases triglyceride levels.

Obesity or visceral fat – Particularly dangerous when concentrated around the abdomen.

Type 2 diabetes or prediabetes – Insulin resistance drives fat storage in the liver.
High cholesterol or triglycerides
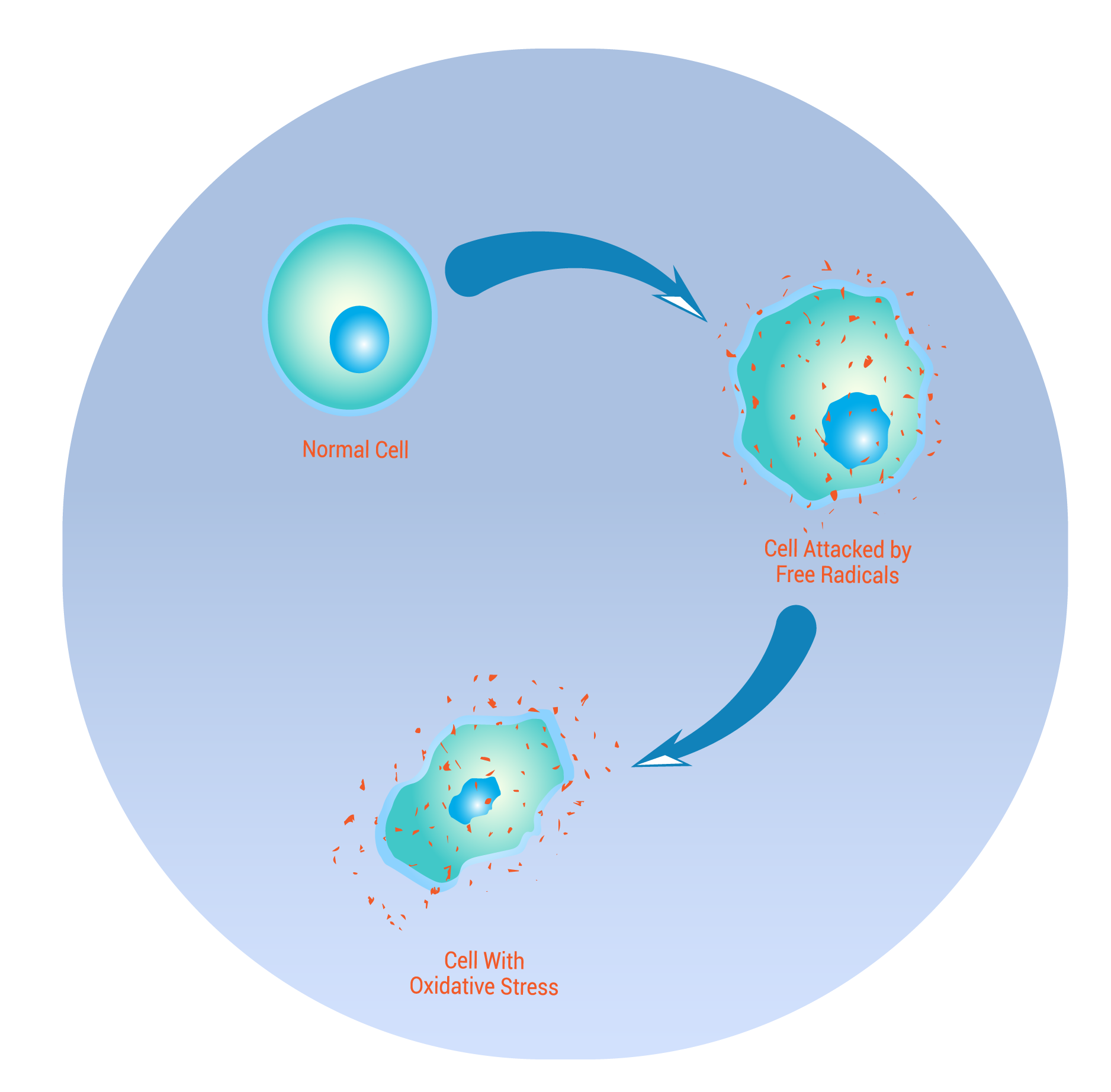
Chronic inflammation or oxidative stress

Polycystic ovarian syndrome (PCOS) – Hormonal imbalance may contribute to liver fat.
Treatment Options for Steatosis
Treatment varies depending on the cause (alcoholic vs. non-alcoholic) and severity.

Medical Interventions
- Weight management – A 5–10% reduction in body weight may significantly improve NAFLD.
- Blood sugar control – Essential in diabetic patients.
- Cholesterol-lowering medications – Statins may be prescribed.
- Vitamin E – Sometimes used as a supplement to reduce liver inflammation (under medical guidance).
Regular Monitoring
- Liver enzyme testing
- Ultrasound or MRI imaging
- FibroScan for liver stiffness
- Biopsy in advanced or uncertain cases
Early detection is key—when caught early, steatosis is treatable, manageable, and often reversible.
So Much Is Still Unknown
Although scientists understand many risk factors, there is still more to learn about why some people develop steatosis while others don’t. Research into genetic susceptibility, microbiome influence, and early biomarkers is ongoing.
What’s clear is that liver health is foundational to overall vitality. A damaged liver doesn’t just affect digestion—it impacts hormones, immunity, mental clarity, and energy.
If you’re at risk—or already living with fatty liver disease—speak to your healthcare provider. Early lifestyle shifts can make all the difference.
Build Me a Meal Plan
Every liver is unique, and so is your lifestyle. That’s why we’ve designed personalized liver-supportive nutrition checklists and recipes to match your tastes and needs.
Further Reading on Steatosis
Mayo Clinic: Fatty Liver Disease Overview
A comprehensive look at symptoms, causes, diagnosis, and treatment options for fatty liver.
https://www.mayoclinic.org/diseases-conditions/nonalcoholic-fatty-liver-disease/symptoms-causes/syc-20354567
Cleveland Clinic: Nonalcoholic Fatty Liver Disease (NAFLD)
Details on risk factors, stages (including NASH), and how to manage or reverse liver fat through lifestyle changes.
https://my.clevelandclinic.org/health/diseases/15831-fatty-liver-disease-nafld
StatPearls – NCBI Bookshelf: Nonalcoholic Fatty Liver Disease
An in-depth clinical resource on NAFLD, NASH, pathophysiology, and treatment, used by medical professionals and researchers.
https://www.ncbi.nlm.nih.gov/books/NBK513253/
PubMed Central: Nutritional Approaches to NAFLD Management
A research review exploring how food, vitamins, and lifestyle impact disease progression.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9192855/
NIH: Exercise for Fatty Liver – Effects on Liver Fat and Inflammation
Summarizes clinical studies showing how aerobic and resistance exercise reduce hepatic fat.
https://pubmed.ncbi.nlm.nih.gov/32167677/
NIH: Gut Microbiota and NAFLD – The Gut-Liver Axis
Explores how imbalances in gut bacteria contribute to liver fat accumulation and inflammation.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7825895/






