Diabetes: What It Is, Why It Happens & How We Can Care for It
Diabetes isn’t just about sugar—it’s about how the body transforms food into fuel and how that process can get stuck, strained, or short-circuited. At its core, diabetes is a condition where the body struggles to use glucose (sugar) as energy because insulin—our glucose “key”—isn’t doing its job.
Sometimes the pancreas doesn’t produce insulin at all. Sometimes it produces plenty, but the body doesn’t respond to it. And in either case, glucose builds up in the bloodstream, where it doesn’t belong. Over time, that build-up can wear down blood vessels, nerves, and organs.
But here’s the truth: diabetes isn’t a personal failure. It isn’t just “too much sugar.” It’s layered. And while genetics can plant the seed, lifestyle, food systems, and chronic stress can water it.
Understanding the Two Main Types
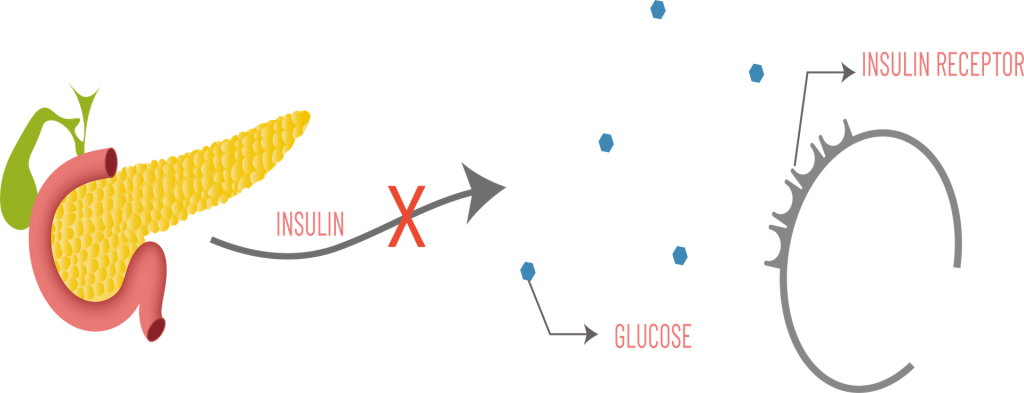
Type 1 diabetes happens when the body’s immune system mistakenly attacks the insulin-producing beta cells in the pancreas. It usually shows up in childhood or young adulthood, often suddenly. There may be a viral trigger. Or an autoimmune one. It’s no one’s fault—and it’s not preventable.
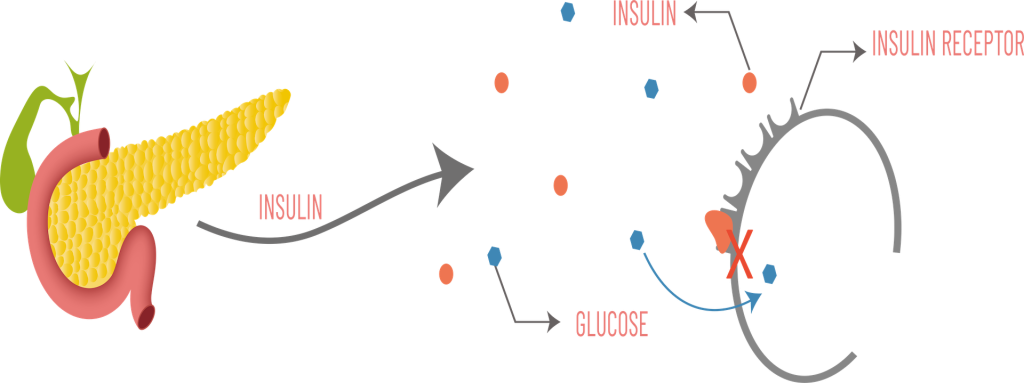
Type 2 diabetes is more common and often develops over time. In this form, the body still makes insulin—but it doesn’t respond to it well. Over time, the pancreas may struggle to keep up. This type is closely tied to chronic inflammation, poor sleep, ultra-processed foods, and a sedentary lifestyle—all realities shaped by culture and circumstance, not just willpower.
There’s also impaired glucose tolerance (IGT)—a sort of early warning system. Not quite diabetes. But not optimal either. IGT often comes with no symptoms at all, which is why so many people live for years not knowing their blood sugar is too high.
The Body’s Signals: Symptoms to Watch For
People with diabetes—especially type 1—can experience sudden drops (hypoglycemia) or dangerous spikes (hyperglycemia) in blood sugar.
Symptoms of Type 1:
Frequent urination, bedwetting (in children who previously stayed dry)
Symptoms of Type 1:
You may feel thirsty, nauseated, tired, or unable to keep fluids down
Symptoms of Type 1:
Weight loss despite eating normally

Symptoms of Type 1:
Constantly hungry

Symptoms of Type 1:
Blurred Vison, Nausea

Symptoms of Type 1:
Fatigue
The Rollercoaster: Blood Sugar Extremes
The goal isn’t to fear these fluctuations—but to understand them and build rhythms that help us stay steady.
Root Causes & Risk Factors
There’s no one reason someone develops diabetes—but we know some patterns.
- Genetics: a strong family history increases risk
- Body weight & fat distribution: especially abdominal fat
- Diet low in fiber & high in refined carbs
- Sedentary lifestyle
- Sleep deprivation & chronic stress
- Gestational diabetes or PCOS history
It’s not about blame—it’s about recognizing patterns, breaking cycles, and finding support without shame.

Diagnosis & Testing

A diagnosis usually begins with a blood test. These include:
- A1C (average blood sugar over 3 months)
- Fasting blood glucose
- Oral Glucose Tolerance Test (OGTT)
- Urinalysis (may detect glucose or ketones early)
Millions of people walk around undiagnosed. It’s worth checking—especially if you feel “off” in ways you can’t explain.
Complications (When It’s Left Untreated)
Without care, high blood sugar can silently damage:
- Eyes (leading to blindness)
- Kidneys (potentially causing failure)
- Nerves (especially in the feet)
- Heart & blood vessels (stroke, heart attack)
- Immune function (leading to chronic infections)
But this isn’t inevitable. With attention, support, and steady habits, complications can be slowed or avoided altogether.
What Helps: Food, Movement, and Rhythm
There’s no one “diabetes diet.” But here’s what helps most bodies:
Food
- Prioritize fiber-rich carbs: leafy greens, beans, oats, quinoa
- Pair carbs with healthy fat or protein
- Minimize ultra-processed snacks and added sugars
- Eat at regular intervals to avoid spikes and crashes
Movement
Move your body daily, even gently
🧪 Monitoring
- Track how food, stress, sleep, and activity affect your numbers
- Use finger-stick meters or continuous glucose monitors (CGMs) if needed
- Talk with your care team about targets and patterns
💊 Medication
Sometimes lifestyle changes aren’t enough on their own. Options include:
- Metformin
- Insulin injections or pumps
- GLP-1 receptor agonists (which may help with appetite and weight)
- Others depending on your needs and health history
There’s no shame in using medication. Support is support.
Community, Compassion, and Healing
Diabetes care isn’t just about numbers. It’s about:
- Learning to listen to your body
- Releasing shame or blame
- Building sustainable habits instead of short-lived rules
- Connecting with a care team that sees you—not just your labs
You are more than your diagnosis. You are worthy of joy, energy, and ease.
📚 Further Reading on Diabetes Health
Chromium and Blood Sugar Regulation – NIH Office of Dietary Supplements
Scientific review of chromium’s role in glucose metabolism and potential supplementation benefits for insulin resistance.
Source: NIH ODS: Chromium & Glucose Metabolism
Diabetes Overview – Mayo Clinic
Comprehensive guide covering the types of diabetes (type 1, type 2, gestational), symptoms, complications, and lifestyle approaches to prevention and management.
Source: Mayo Clinic: Diabetes
Diabetes: Types, Causes & Treatments – Cleveland Clinic
In-depth explanation of risk factors, blood sugar monitoring, medication options, and lifestyle changes to help manage diabetes effectively.
Source: Cleveland Clinic: Diabetes
Diabetes Mellitus – StatPearls (NCBI Bookshelf)
Clinical review on diabetes pathophysiology, diagnosis, complications, and current treatment strategies. Designed for healthcare professionals and advanced readers.
Source: NCBI Bookshelf: Diabetes
Lifestyle Management of Type 2 Diabetes – PubMed Central
Evidence-based research highlighting the role of diet, movement, sleep, and stress reduction in improving insulin sensitivity and glycemic control.
Source: PMC: Lifestyle Management of Type 2 Diabetes
Dietary Approaches to Managing Diabetes – PubMed Central
Study comparing different dietary patterns (low-carb, Mediterranean, plant-based) in relation to A1C levels, insulin resistance, and inflammation.
Source: PMC: Dietary Approaches to Diabetes